Capella NURS-FPX6011 Assessment 1 EBP Assignment Example
Part 1: Concept Map
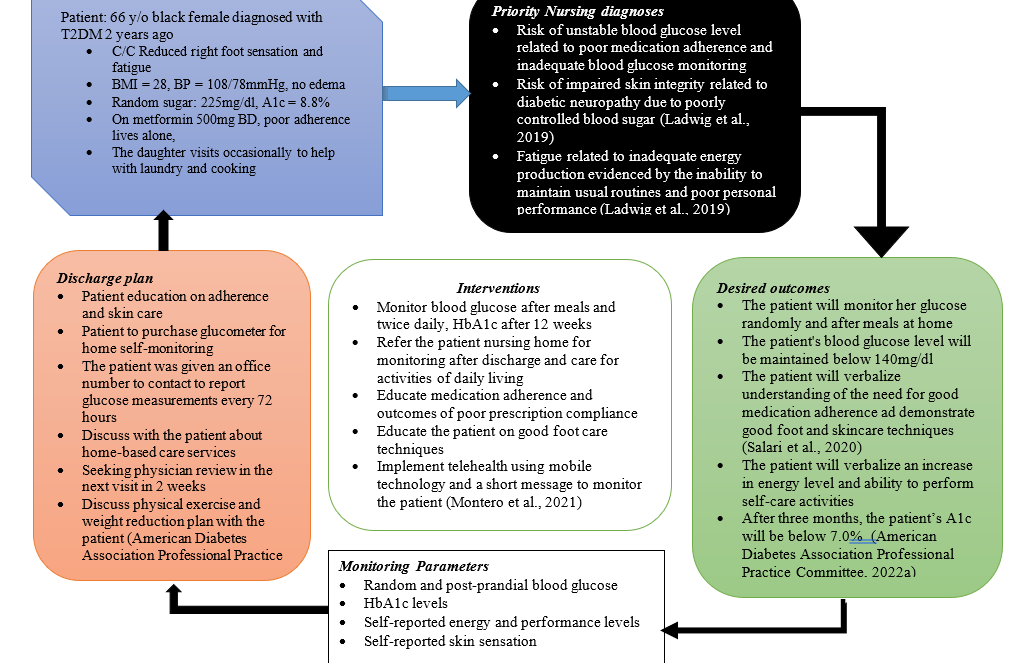
Part 2: Supporting the Concept Map
The development of this concept map was guided by the nursing process. This patient came into the office with a chief complaint of reduced sensation on the right foot that was on and off but mild in functional limitation. The assessment revealed no other symptoms related to renal, ophthalmic, gastrointestinal, or cardiac complications of diabetes. The purpose of this narrative review of the concept map is to describe how evidence-based practice influenced this concept map and care plan in terms of analysis of the patient’s needs, communication with the patient and her family, and the value of the evidence-based sources used.
Patient Needs Analysis
During this visit, the patient’s main concerns were the reduction of right lower limb and foot sensation and fatigue. On further probing, the assessment found that this patient’s compliance with her metformin has been erratic and her socioeconomic circumstances could have also contributed to her current situation. She has missed most of her doses in the past few months because her daughter, who used to remind her to take her pills, moved to another state for permanent employment and has been held up with work lately.
The patient is retired; thus, her primary source of income is through her son and daughter, who are both employed. Her children are both married but still find time to come and visit. This patient is a staunch Christian believer and she reports that her faith has kept her through to this time. This might have contributed to the reluctance to comply fully with her prescription. Nevertheless, this patient’s cultural and socioeconomic needs greatly influenced the development of this concept map and the care plan.
The patient lives alone; thus, this care plan instituted monitoring strategies to ensure that the patient achieves self-care by improving her fatigue. Priority was given to stabilizing blood sugar levels and improving adherence to ensure that her metabolic demands were met. Monitoring through telehealth and mobile technology was a vital part of this plan because it would enable remote management of the patient through enhanced follow-up after short time intervals. In the discharge plan, the patient was helped to create a plan that included an alarm to remind her about her medication time and times to record her blood glucose to report three days later.
The development of the patient was also influenced by her identity and cultural needs. As an African American, she is at risk of cardiovascular diseases such as heart failure. Therefore, an assessment of her blood pressure and cardiovascular complication, such as lower limb edema from heart failure and acute kidney injury, was justified for this patient. This patient is overweight (BMI=28), which adds to her cardiovascular risk. Therefore, the inclusion of exercise and a weight reduction plan through diet were discussed during a motivational interviewing session.
The interventions were driven at meeting care needs illustrated in the three priority diagnoses. Most of the desired outcomes of these interventions were intertwined and such that more than one intervention could be used to meet a single outcome. Therefore, I included the monitoring outcomes measurement parameters that would be discussed with the patient during every review session after every 72 hours. The patient’s family was included in this plan through her daughter, who accompanied her to the office. She desired to treat her mother from home even if it meant that the care costs would increase. Therefore, I added community resources such as home-based care interventions to improve this patient’s self-care at home.
Communication Strategies.
The communication plan with this patient and her family will involve both remote and face-to-face communication. Remote communication through telehealth would help monitor patient progress and scheduling appointments. After every four weeks, the patient would revisit the officer for physical assessment and face-to-face communication. To ensure that these communications were honest and productive. The communication times would be scheduled and contents tailored to meet the patient’s care needs.
The patient’s daily readings would be communicated through phone calls but charted on paper to be delivered during physical sessions. This would ensure that only important and useful is shared, but every detail is documented for monitoring and evaluation. The content of the communication with the patient an